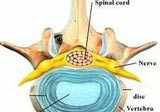
What is a herniated disc?
By Jonathan Cluett, M.D., About.com Guide
Updated March 23, 2012
About.com Health’s Disease and Condition content is reviewed by the Medical Review Board
L5 Bulging Discwww.LaserSpineInstitute.com/Disc
Safe Outpatient Procedure. Back Pain Relief With Minimal Recovery.
Herniated Diskwww.harthosp.org
Causes, Symptoms & Treatment Find a Specialist Near You.
Lumbar Stenosis Treatmentwww.Bonati.com
Minimally Invasive Procedures. Fast Recovery. No Hospitalization.
Dr. Debra Petrucci, Neurosurgeon Board Certified in Neurosurgery
Read About Our 30-Min Treatment.
Get Total Freedom From Back Pain!
Many patients with back pain, leg pain, or weakness of the lower extremity muscles are diagnosed with a herniated disc. When a disc herniation occurs, the cushion that sits between the spinal vertebra is pushed outside its normal position. A herniated disc would not be a problem if it weren’t for the spinal nerves that are very close to the edge of these spinal discs.
What is the spinal disc?
The spinal disc is a soft cushion that sits between each vertabrae of the spine. This spinal disc becomes more rigid with age. In a young individual, the disc is soft and elastic, but like so many other structures in the body, the disc gradually looses its elasticity and is more vulnerable to injury. In fact, even in individuals as young as 30, MRIs show evidence of disc deterioration in about 30% of people.
What happens with a ‘herniated disc’?
As the spinal disc becomes less elastic, it can rupture. When the disc ruptures, a portion of the spinal disc pushes outside its normal boundary–this is called a herniated disc. When a herniated disc bulges out from between the vertebrae, the spinal nerves and spinal cord can become pinched. There is normally a little extra space around the spinal cord and spinal nerves, but if enough of the herniated disc is pushed out of place, then these structures may be compressed.
What causes symptoms of a herniated disc?
When the herniated disc ruptures and pushes out, the nerves may become pinched. A herniated disc may occur suddenly in an event such as a fall or an accident, or may occur gradually with repetitive straining of the spine. Often people who experience a herniated disc already have spinal stenosis, a problem that causes narrowing of the space around the spinal cord and spinal nerves. When a herniated disc occurs, the space for the nerves is further diminished, and irritation of the nerve results.
What are the symptoms of a herniated disc?
When the spinal cord or spinal nerves become compressed, they don’t work properly. This means that abnormal signals may get passed from the compressed nerves, or signals may not get passed at all. Common symptoms of a herniated disc include:
- Electric Shock Pain
Pressure on the nerve can cause abnormal sensations, commonly experienced as electric shock pains. When the compression occurs in the cervical (neck) region, the shocks go down your arms, when the compression is in the lumbar (low back) region, the shocks go down your legs.
- Tingling & Numbness
Patients often have abnormal sensations such as tingling, numbness, or pins and needles. These symptoms may be experienced in the same region as painful electric shock sensations. - Muscle Weakness
Because of the nerve irritation, signals from the brain may be interrupted causing muscle weakness. Nerve irritation can also be tested by examining reflexes. - Bowel or Bladder Problems
These symptoms are important because it may be a sign of cauda equina syndrome, a possible condition resulting from a herniated disc. This is a medical emergency, and your should see your doctor immediately if you have problems urinating, having bowel movements, or if you have numbness around your genitals.
All of these symptoms are due to the irritation of the nerve from the herniated disc. By interfering with the pathway by which signals are sent from your brain out to your extremities and back to the brain, all of these symptoms can be caused by a herniated disc pressing against the nerves.
How is the diagnosis of a herniated disc made?
Most often, your physician can make the diagnosis of a herniated disc by physical examination. By testing sensation, muscle strength, and reflexes, your physician can often establish the diagnosis of a herniated disc.
An MRI is commonly used to aid in making the diagnosis of a herniated disc. It is very important that patients understand that the MRI is only useful when used in conjunction with examination findings. It is normal for a MRI of the lumbar spine to have abnormalities, especially as people age. Patients in their 20s may begin to have signs of disc wear, and this type of wear would be expected on MRIs of patients in their 40s and 50s. This is the reason that your physician may not be concerned with some MRI findings noted by the radiologist.
Making the diagnosis of a herniated disc, and coming up with a treatment plan depends on the symptoms experienced by the patient, the physical examination findings, and the x-ray and MRI results. Only once this information is put together can a reasonable treatment plan be considered.